Airway Clearance & Exercise
Within this section you will find information about various airway clearance techniques, the role of exercise in CF, tips to save energy and fight fatigue, how we measure functional status using a 6-minute walk test and how to cope with shortness of breath.
Physiotherapy
There are several physiotherapists on the CF team and they cover both the inpatient ward and outpatient clinic.
Physiotherapy is a healthcare profession which aims to promote, improve and maintain mobility and physical functioning ultimately optimizing quality of life. Physiotherapists can help people with a wide range of conditions ranging from a sprained ankle to patients that have had stroke or are managing chronic conditions like diabetes or CF. All physiotherapists are registered to practice in Canada and have met national entry-level education and practice standards. They have also successfully passed a standardized physiotherapy competence examination prior to being registered with the College of Physiotherapists in their province/territory. Physiotherapists combine their in-depth knowledge of the body and how it works with specialized hands-on clinical skills to assess, diagnose and treat symptoms of illness, injury or disability. To learn more about physiotherapy, visit the Canadian Physiotherapy Association.
Saving Energy & Fighting Fatigue
Feeling tired and as though you are unable to do things can sometimes happen in CF. While this can be frustrating, it is important to know that asking for help is more than okay. In addition, there are many tips and tricks you can do in your daily life to help reduce feelings of tiredness, and be able to perform routine tasks a little easier.
For more information on energy conservation, explore this handout from our clinic physiotherapists.
Coping With Shortness of Breath
Shortness of breath can occur due to the airways being plugged with mucous. If you feel short of breath, try the following steps from the Lung Association.
Remember: Breathlessness on effort is uncomfortable but not in itself harmful or dangerous.
- STOP and REST in a comfortable position.
- Get your head down.
- Get your shoulders down.
- Breathe IN through your MOUTH.
- Blow OUT through your MOUTH.
- Breathe in and out as fast as necessary.
- Begin to BLOW OUT LONGER, but not forcibly, and use pursed lips if you find it effective.
- Begin to SLOW your breathing.
- Begin to use your nose.
- Begin diaphragmatic breathing.
- STAY IN POSITION for 5 minutes longer.
Source: The Lung Association
For more infomation, read this handout on coping with breathlessness.
Chest Physiotherapy (also called ‘Airway Clearance’)
Chest physiotherapy is a broad term used to describe a variety of manual and breathing techniques that help your body to clear mucous from your lungs. Chest physiotherapy can also improve the movement of air into and out of your lungs, as well as decrease shortness of breath and fatigue associated with the increased work of breathing often experienced by people with CF. Daily airway clearance is standard of care for people with CF.
Exercise
Six Minute Walk Test
Six minute walk test (6MWT) is a standardized functional test designed to assess an individual’s functional capacity. Functional capacity refers to how able someone is to perform tasks and activities that they find necessary or desirable in their lives. When an individual is sick, their ability to function may be affected; but as one gets better, they may regain their ability to function. The only way we can accurately tell your level of functional capacity is to perform a functional test, like the 6MWT.
During a 6MWT, you are asked to walk as far as possible in six minutes on a set route. If necessary, you will be asked to use adequate supplemental oxygen as recommended by the respiratory therapist during the walk. We will measure your oxygen saturation, heart rate, your perceived breathlessness and fatigue before and after the test, and the amount of rest you need during the test. The distance you covered over the six minutes will be recorded. Studies have shown that the distance walked in the 6MWT significantly increases in the first two trials but reaches a plateau by the third trial. Thus, the third trial result will give the most accurate indication of level of functional capacity.
Research studies have shown that the distance you walk during the 6MWT is directly proportional to:
- Your exercise tolerance
- Your maximal oxygen consumption (VO2max – the amount of oxygen delivered to your active body tissues, indicating your fitness level)
- Your lung function
- Your feeling of breathlessness
Six minute walk test can provide information about your level of daily activity, your well-being, and functional exercise tolerance that you need to perform your daily activities.


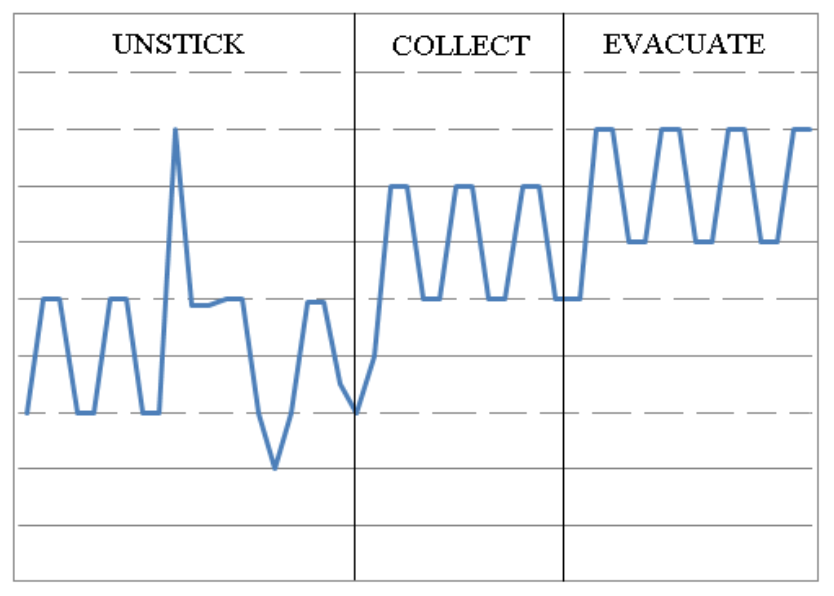 This is a complicated airway clearance technique to learn and perform. It should be carefully taught and reviewed by one of the physiotherapists on the CF team.
This is a complicated airway clearance technique to learn and perform. It should be carefully taught and reviewed by one of the physiotherapists on the CF team.