Breathing Gear
In this section, read more about equipment such as nebulizers and compressors, learn how to clean them, how to prepare your therapy, and about the various types of oxygen. Understanding your equipment is important for proper use of medication and staying healthy!
Nebulizers & Compressors Overview
Air compressors are machines that force room air into a smaller volume, thus increasing the air pressure, to create a stream of air. Air compressors are used with a nebulizer to convert liquid medication to a fine mist that can be inhaled.
Patients who are eligible for the Assistive Devices Program (ADP) have 75% of the cost of the air compressor covered with an application signed by the CF doctor. You are eligible for ADP if you have a OHIP card and require the use of equipment for at least 6 months, regardless of your income. If you have private insurance, your plan may cover the total cost of an air compressor.
Air compressors can be purchased at ADP authorized vendors such as Medigas, Pro Resp, Vital Air, Complete Oxygen Care, MedPro. Below are pictures of recommended compressors. The Devilbiss Pulmo Aide is a very reliable compressor. If you do not purchase from an ADP authorized vendor you will not be able to submit an application for funding.
Compressors have filters that should be changed regularly (every 3 months or more if home is very dusty). Filters can be purchased at the same place as the compressor. Check the filter on your compressor monthly and replace it as per manufacturer’s specifications.
These compressors cannot be used outside of North America due to voltage differences.
Compressors are under warranty for 5 years. If there are any problems with the compressor, return to the vendor from which it was purchased. Check the filter on your compressor every month and replace it according to the manufacturer’s specifications.
For a new compressor after the 5 year warranty has elapsed and the compressor is no longer in good working condition – you will have to provide evidence of repair bills etc, in order to receive ADP funding again.
Mid Range Compressors
DeVilbiss PulmoAide

- Max operating pressure 35 psi
- Maximum Liter Flow 8 lpm
- 9 lpm or greater
DeVilbiss Compact

- Most recommended
These compressors cannot be used outside of North America
For ventolin and atrovent treatments, any re-usable nebulizer that can be washed and disinfected on a daily basis can be used. These are available at the companies listed above.
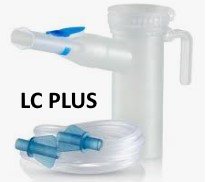
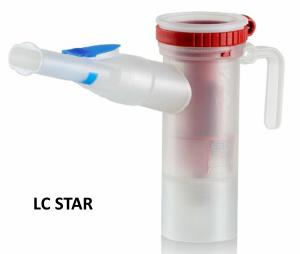
For inhaled antibiotic and/or mucolytics, we recommend using one of the Pari reusable nebulizer with mouthpiece. It is designed to improve aerosol delivery to the small airways. Treatment times may be as quick as 10 minutes or as long as 20-30 min depending on the volume being nebulized. They can be cleaned in the dishwasher or boiled to disinfect. If rinsed and cleaned on a daily basis, these nebulizers will last up to 6 months. At this time they should be replaced. The cost is $22.00, and can be purchased at the St. Michael’s Hospital outpatient pharmacy. The Pari nebulizers are: Pari LC sprint, Pari LC plus, Pari LC star.

Nebulizers & Compressors FAQs
A nebulizer is a device commonly used to administer medication in the form of a mist that is inhaled into the lungs. The most commonly used nebulizers are called Jet nebulizers. Jet nebulizers are connected by a piece of tubing to a compressor.
A compressor is a device that drives the nebulizer. It compresses room air and blasts it at a high speed through a liquid medicine to turn it into a mist of fine droplets which is then inhaled by the individual.
A mouthpiece is a preferred method of delivering aerosol to the airway, regardless of age. A mouthpiece delivers more drug to the airway with less waste than a mask. A mask should only be used when a mouthpiece is not tolerated.
Nebulizer treatment times will vary considerably depending on many factors including:
- Type of nebulizer being used
- Type of compressor being used
- Persons breathing characteristics
- Type of drug being nebulized
- Amount of drug being nebulized
- Temperature and relative humidity
In general, most PARI Jet nebulizers (LC Sprint, LC Plus & LC Star) will deliver 2.5mL of saline solution in 5 to 8 minutes.



Note: Treatment times for most CF medications will be longer as there is typically a larger volume of the drug being nebulized and the drugs are generally thicker.
If there is no mist coming out of your nebulizer it probably means that your compressor isn’t functioning properly or that particles too small for you to see have attached themselves to key parts of the nebulizer mechanism and are preventing it from working properly. Perform the following:
- Clean and disinfect your nebulizer following the instructions provided under Cleaning and disinfecting your nebulizer.
- Ensure your nebulizer is assembled according to the manufacturer’s instructions.
- Ensure that the filters on your compressor are clean and replaced regularly.
- Confirm that flow is being produced from your compressor when it is turned on.
If none of these interventions work, you may need to contact the manufacturer or your health care provider for further assistance.
Replacing Nebulizers
Nebulizers should be replaced on a regular basis. Your PARI nebulizer should last from 6 months to 1 year with general use. If treatment times are taking longer, replacing the nebulizer may help. It is recommended that you buy a back-up nebulizer in case your nebulizer becomes lost, damaged or soiled.
Replacing Compressors
Compressors need only be replaced when they stop functioning or when their performance results in decreased drug delivery to the lungs. The Ontario Ministry of Health and Long-Term Care Assistive Devices Program (ADP) currently offers funding assistance for a new compressor every 5 years if it is not in good working condition. You should always contact the vendor from where you purchased the compressor if you have any problems with it.
Important Note: A good general rule is to replace the Air Filter every 6 months. You must replace the filter immediately if it gets wet or becomes clogged.
In Ontario, individuals with CF who require regular, long-term treatment (for 6 months or longer) with inhaled aerosolized medications, qualify for funding assistance of their medication compressor. Funding assistance is equal to 75% of the vendor’s selling price up to a maximum amount. Assistance is provided by the Ontario Ministry of Health and Long-Term Care Assistive Devices Program (ADP).
Note: Nebulizers are not currently covered by this program.
Nebulizers
You can buy a nebulizer at the St Michael’s Hospital Pharmacy. Prices are approximately $25.00. Be sure to ask your Respiratory therapist for more information on buying nebulizers.
Compressors
You can buy compressors directly from the vendor. Here is a list of approved respiratory equipment vendors from the Ministry of Health and Long Term Care from which you can buy compressors from.
If you have more questions, ask your respiratory therapist.
Treatment Best Practices
Follow these steps when preparing your treatment:
- Wash your hands thoroughly with soap and water. This helps to prevent infection.
- Place the compressor on a clean surface and connect it to a power supply.
- Attach the long connecting tubing to the air out port of the compressor.
- Take out your nebulizer and remove the nebulizer top from the nebulizer cup. Place the top on a clean surface.
- Check the expiration date of the medication you will be nebulizing.
- Empty the medication as instructed into the nebulizer cup. It is very important that you use the full dose of the drug.
- Replace the nebulizer top back onto the nebulizer cup.
- Connect the mouthpiece to the nebulizer.
- Attach the free end of the long connecting tubing to the port on the bottom of the nebulizer. Keep the nebulizer held upright so as not to spill any of the medication.
- Turn on the compressor and check to see that a mist is coming out of the nebulizer.
Note: For some inhaled medications it is necessary to do a quick breathing test to make sure you tolerate the medication before it is prescribed. Your first treatment should be performed under the guidance of a Physiotherapist or Respiratory Therapist to ensure proper technique and correct use of equipment.
Follow these steps to make sure you are taking your treatment properly:
- Sit upright in a chair and place the mouthpiece of the nebulizer between your teeth and on top of your tongue. Be sure not to block the airflow with your tongue.
- Breathe normally by inhaling and exhaling through your mouth. Do not breathe through your nose. If you have difficulty breathing through your mouth, try using a nose clip.
- Every 1–2 minutes take a couple of deep breaths through the mouthpiece to help increase the amount of medication delivered to the small airways in your lungs.
- Do not be concerned if condensation collects in the long connecting tube during your treatment.
- When the nebulizer begins “spitting”, gently tap the nebulizer cup and continue breathing until the nebulizer cup is empty, or stops producing a mist.
- It is important to inhale the full dose of your treatment. If you are interrupted, or begin coughing during your treatment, turn off the compressor so as not to waste the medication.
- To resume your treatment, turn the compressor back on and continue.
- If you detect a leak, or feel any moisture coming from the nebulizer during treatment, turn off the compressor and check to see that the nebulizer cap is correctly sealed before continuing.
Important Notes About Mouthpieces:
- A mouthpiece is the preferred method of delivering aerosol to the airway, regardless of age.
- A mouthpiece delivers more drug to the airway with less waste than a mask.
- A mask should only be used when a mouth piece is not tolerated.
Germs can grow on or in anything that is wet, including your nebulizer. The Cystic Fibrosis Foundation consensus guidelines currently recommend that nebulizer equipment be cleaned, disinfected, rinsed, and air-dried between uses.
This video demonstration is for the Altera and eFlow Nebulizers. This same technique can also be used for other PARI nebulizers.
To Clean And Disinfect Your Device, Follow These Steps:
- Rinse your device with water immediately after use. This will stop any debris such as drugs, spit and mucous from sticking to the inside of the device.
- Clean your hands.
- Disassemble the device.
- Wash parts with mild soap and warm water. DO NOT WASH THE TUBING. Ensure you only use clear (non-opaque) soap for cleaning the metal aerosol head on the eflow.
- Use a small scrub brush or cloth to remove any debris. Take care not to tear or break any of the pieces. Do NOT use a scrub brush on the metal eflow aerosol head.
- Rinse all parts well with sterile water.
- Use one of the following methods to disinfect your equipment:
- Boil for 10 minutes. Fill a clean pot with enough water to cover all of the pieces. Bring the water to a boil then place all pieces into the boiling water for 10 minutes. Do not forget to remove the equipment after 10 minutes. If the water evaporates, the plastic will melt onto the pot.
- Microwave at 2.45 Ghz for 5 minutes. Place pieces in a microwavable bowl covered with water. Do not microwave the PARI eFlow, as this nebulizer contains metal parts.
- Dishwasher at temperature > 158°F (70°C) for 30 minutes. To obtain this temperature, the dishwasher water may need to be reset.
- Soak in 3% hydrogen peroxide for 30 minutes. After removing from the peroxide, rinse well with sterile water. Do not use bottled, distilled or tap water as these may contain germs. Tap water can be made sterile by boiling it for 10 minutes. Use this water once and then throw it out.
- Electric steam sterilizer such as a baby bottle steam sterilizer. Counter top version, NOT microwave version as some nebulizers (eflow Altera) has metal parts.
- Soak in 70% isopropyl alcohol for 5 minutes. Ensure all pieces are totally submerged. Rinse well with sterile water. Tap water can be made sterile by boiling it for 5 minutes.
- Remove pieces carefully and air dry the equipment on a clean, dry, lint-free towel and cover.
- Reassemble the equipment when the parts are dry and store.
Remember:
- Check the filter on your compressor every month and replace it according the manufacturers specifications.
- Replace your nebulizer every 6 to 8 months and your compressor every 5 years.
- Germs will grow on or in anything that is wet.
Oxygen Therapy
Individuals with lung disease can have low levels of oxygen in their bodies and some need to use extra (supplemental) oxygen to bring their oxygen levels up to a healthier level. Some people with Cystic Fibrosis may require supplemental oxygen. Supplemental oxygen protects the body from the effects of low oxygen levels. It also helps your body to function better and allows you to stay more active.
Oxygen is a basic need for all humans. The air we breathe contains about 21% oxygen. This amount is enough for people with healthy lungs but may not be enough for some people with lung disease. These individuals require extra oxygen to maintain normal bodily function.
A healthcare provider will figure out if you need oxygen therapy by testing the amount of oxygen in your blood. This can be done with a test called an arterial blood gas (ABG). An ABG involves taking a sample of blood from an artery (usually in the wrist). Your oxygen level (oxygen saturation) can also be measured with a small device called a pulse oximeter. This device can be clipped painlessly onto your finger, toe or earlobe. With this device your oxygen levels can be checked over a period of time, for example, during sleep or exercise. The general treatment goal is to keep your oxygen at a level that meets the body’s need for oxygen, usually 88% or above.
Oxygen is considered a drug and requires a prescription from your healthcare provider. The amount of oxygen that you need may be different depending on the type of activity you are doing. It is very important that you use the amount of oxygen that has been prescribed to you for each activity. Using too little oxygen may starve your brain and heart of oxygen, resulting in fatigue, memory loss, and changes to the heart. Too much oxygen can also cause problems.
During sleep, people slow down their breathing. People who have low oxygen levels while awake will usually also have low oxygen levels during sleep. In some cases, patients who may not require oxygen while awake may need extra oxygen while sleeping. Your healthcare provider will determine how much oxygen you should use at night.
During physical activity people use more energy and consequently need more oxygen. To find out how much oxygen is needed during activity, the healthcare provider will perform an exercise, or walking, oximetry. During this test your oxygen saturation is monitored throughout and your supplemental oxygen is adjusted to the appropriate level.
Some individuals only need oxygen when they are active or while sleeping, however, in most cases, oxygen should be used 24 hours a day. Talk to your CF Respiratory Therapist to see what is right for you.
Some individuals may only need to use oxygen during a disease flare-up or infection and are able to stop its use when their condition improves. Other individuals may need to continue oxygen therapy to treat a chronic illness. You should never make changes or stop your oxygen therapy without first consulting your healthcare provider.
Oxygen Concentrators
Oxygen concentrators produce oxygen by taking in room air and sifting out the oxygen. Concentrators are powered by electricity. Because oxygen concentrators make their own oxygen, they do not need to be replaced or refilled regularly. Concentrators may be portable or stationary. Portable Oxygen Concentrators (POC’s) run off of a small battery and are typically used outside of the home, while stationary concentrators are plugged into the wall and are used inside the home.
Oxygen Cylinders
Oxygen cylinders are metal tanks that contain oxygen compressed under high pressure. Oxygen cylinders lose oxygen only when they are used. They come in a variety of different sizes.
Liquid Oxygen
Liquid oxygen is made by super-cooling oxygen gas, which changes it to a liquid form. The liquid turns back into a gas before leaving the container and remains as a gas when it is breathed in. Oxygen in liquid form takes up much less room and can be stored in a special thermos called a reservoir. Portable units are filled from a reservoir for travel and use outside the home. Liquid oxygen systems lose oxygen even when they are not in use.
Oxygen Conserving Devices
Many oxygen systems deliver oxygen continuously (while you inhale and exhale). Oxygen conserving devices are used with your oxygen delivery system to make the delivery of oxygen more efficient by reducing the amount of oxygen that is wasted during exhalation. Conserving devices allow your oxygen supply to last longer. This may cut down on the number of deliveries required by your oxygen vendor and extend the life of your portable unit.
Oxygen is a treatment and, like any other treatment, there are safety considerations you need to know about. Read below to learn more.
Oxygen Is A Drug
The use of oxygen requires a prescription from your healthcare provider. It is very important to use the amount of oxygen that has been prescribed to you. Either too little or too much oxygen can be a problem. If you have symptoms of drowsiness, morning headaches, fatigue or breathlessness, you need to contact your healthcare provider.
Fire Safety
- Oxygen does not burn by itself but will make a flame hotter and burn more vigorously.
- Oxygen systems should be kept at least 6 feet (2 meters) away from sources of heat or open flame.
- Never smoke or be around other people that are smoking while wearing oxygen.
- Smoking while wearing oxygen is a serious fire hazard and can cause your nose, hair, and clothing to catch fire.
- Ask others to not smoke while visiting you.
- The local fire department should be informed that you have oxygen in your home.
- Signs should be posted wherever oxygen is being used. Ask your vendor for a sign.
Oxygen Must Be Handled Carefully
- Oxygen must be stored in a well-ventilated area of the house.
- Do not store cylinders or liquid units in a closet.
- Ensure cylinders are well secured at all times.
- Frost injuries to the skin can occur when filling portable liquid oxygen tanks from larger units.
- Ask the person delivering the liquid oxygen to watch you fill your portable liquid unit to make sure you are doing it correctly.
Oxygen Conserving Devices Aren’t For Everyone
Conserving devices can be useful under some circumstances but if you tend to breathe through your mouth while using a conserver you may not be getting the right amount of oxygen. Talk with your vendor and healthcare provider when considering the option of a conserving device.
Ontario residents who have an illness resulting in the need for long term oxygen therapy. Applicants must have a valid Health Card and meet the medical criteria.
Do I Have To See My Doctor?
Yes, your health care provider will order a test to check your oxygen levels. The results of this test will help them decide if you meet the Home Oxygen Program medical criteria.
How Do I Apply?
You and your health care provider must fill out a Home Oxygen Program Application form. This form must be given to an oxygen vendor (supplier) and is then sent to the Ministry’s Home Oxygen Program. It is very important that this form be filled out correctly.
How Will I Get My Oxygen Equipment?
Your oxygen vendor can show you the different types of oxygen systems available. A list of registered vendors can be obtained from the Home Oxygen Program at (416) 327-8804 or toll free at 1-800-268-6021. Registered vendors agree to follow Home Oxygen Program policies. They must not charge more than the Program-approved price for the oxygen and approved equipment. They may charge less if they choose.
Here is a list of approved home oxygen vendors.
How Much Does The Home Oxygen Program (HOP) Pay?
If you fall within one of these three criteria, the Home Oxygen Program will pay for 100% of the monthly cost of a basic oxygen system according to your oxygen needs.
- 65 years or older
- a recipient of Ontario Works (OW), Ontario Disability Support Program (ODSP), Assistance to Children with Severe Disabilities (ACSD)
- receiving professional services through the Local Health Integrated Network (LHIN)
If you are 64 years or younger, and you are not receiving benefits from OW, ODSP, ACSD, and do not reside in a Long Term Care Facility, the Home Oxygen Program will pay 75% of the monthly cost of a basic oxygen system according to your oxygen needs. You are responsible for paying the remaining 25%. All prices include basic disposable supplies such as masks, nasal cannula, and bubble humidifiers.
Will My Private Insurance Cover Any Costs?
Many private insurance companies will cover any additional costs related to oxygen therapy. If you have private medical coverage, check with them to see if they will pay for additional charges not covered by the Home Oxygen Program.

